March 2011

Introduction
Although Rural Emergency Departments operate 24 hours a day, not all hospital resources can do the same. In order to maximize the number of daytime radiographers, a reduced service is often in place after hours. Deciding to call in a radiographer at night may reduce the number of radiographers available the next day.
Unfortunately there is little research to base out of hours radiology guidelines on. Nobody really knows which images can be safely delayed until morning. The best that can be done is to see what has worked in other rural hospitals.
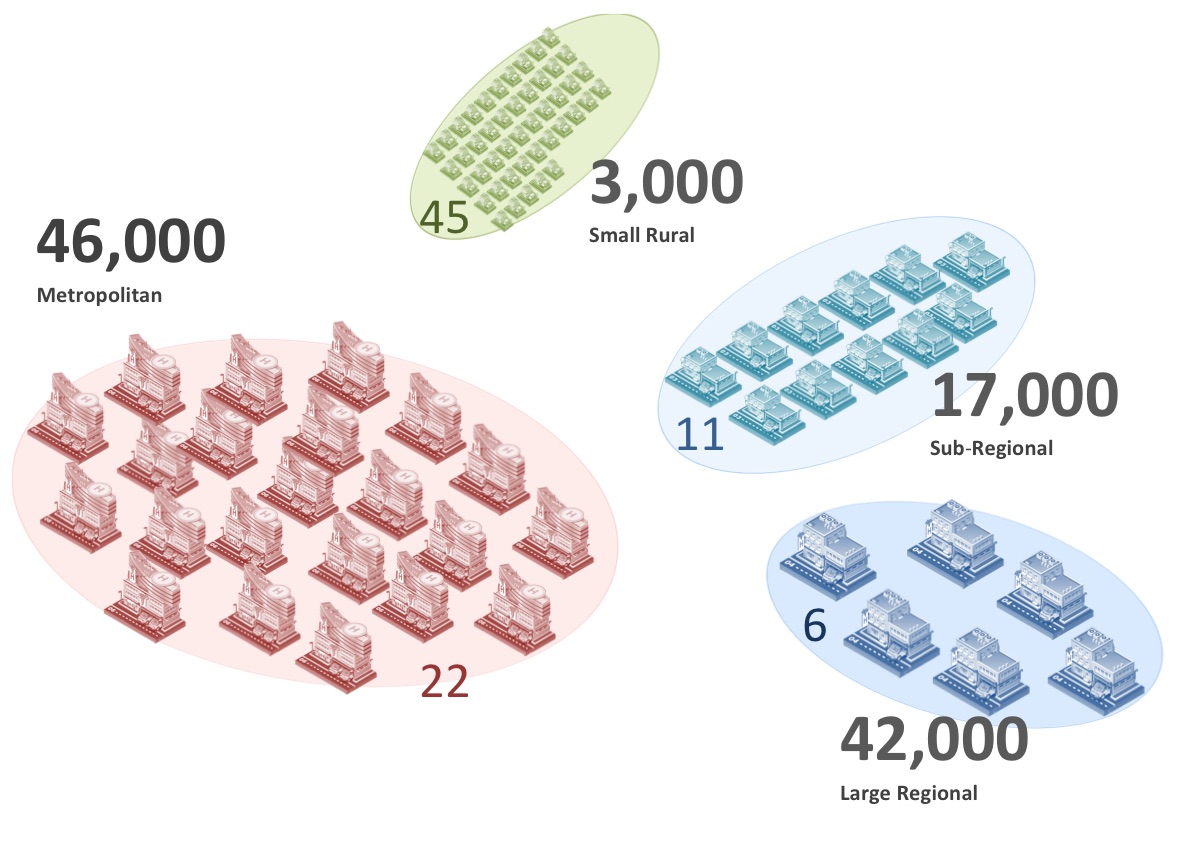
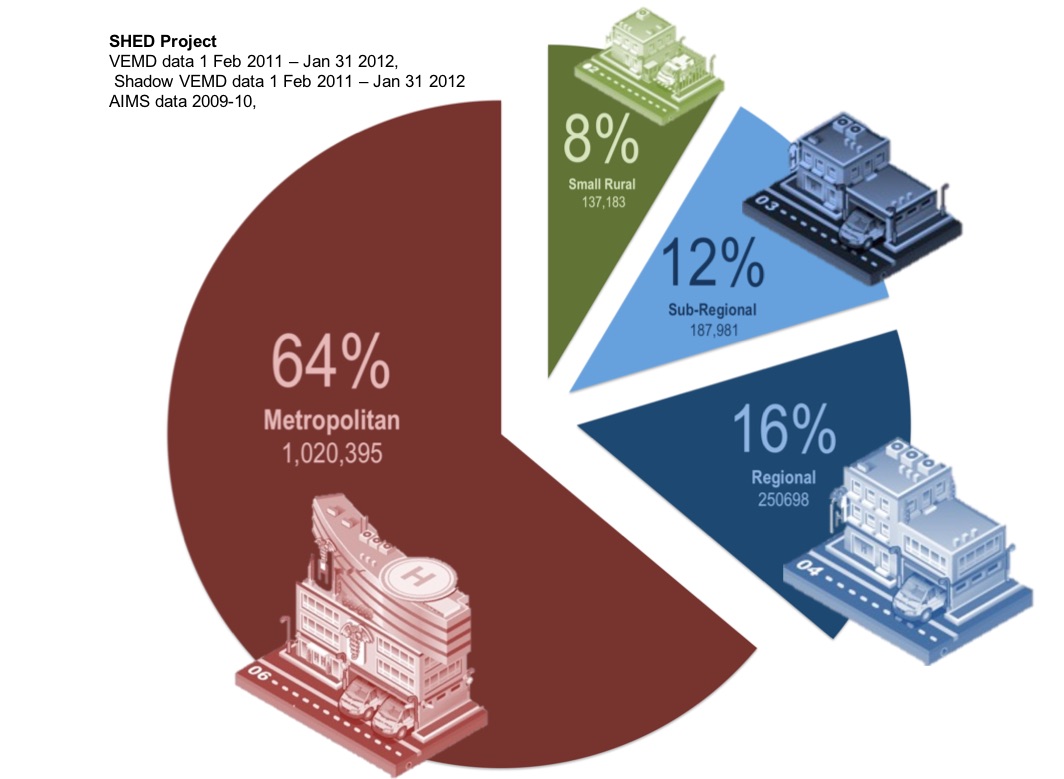
These guidelines were originally written for Portland District Hospital in Western Victoria. Portland is a town of 10,000 people on the South West Victorian coast, four hours drive from the capital city and over one hour drive to the nearest regional centre. The hospital has 69 beds, and the Emergency Department sees 9000 patients annually. The radiology facilities available between nine AM and five PM on weekdays include X-rays, CT scans and ultrasound. The radiographer is on call from home after these hours and on public holidays. There is no onsite radiologist, but opinions are obtainable by telemedicine 24 hours each day.
Principles
Radiographic imaging should only be ordered at night if it will significantly change the management of a patient. Positive images that confirm a diagnosis and negative images that exclude a diagnosis can both be useful. Radiographs should be ordered if a delay in imaging could adversely affect patient outcome. This can occur when uncertain diagnosis or inability to exclude important diagnoses result in
1. Delayed critical treatment
– Example: Confirming air under the diaphragm prior to laparotomy
2. Delayed critical investigation
– Example: excluding asymmetrical ICP rise prior to lumbar puncture
3. Delayed transport to critical care services
– Example: excluding pneumothorax prior to trauma transport by air
4. Delayed transport for urgent surgery
– Example: confirming fracture type underlying open wound
5. Prolonged patient pain because treatment cannot be initiated
– Example: confirming first dislocation of shoulder prior to reduction
6. Prolonged patient pain because treatments cannot be removed
– Example: Many hours in cervical collar when it could be removed if imaging showed no fracture
Approval
Several options are available
1. Emergency department staff can order any image, using this protocol as a guide
2. All image requests have to be cleared by the radiologist
3. Requests in accordance with this protocol can be ordered without radiologist approval. Borderline cases or cases outside the parameters of this guide have to be cleared by a radiologist. This is the option chosen by Portland District Hospital.
Weekends and public holidays
These are officially out of hours, but sometimes it is inappropriate for patients seen on Friday night to wait for two days for their imaging. This is particularly problematic on long weekends. For this reason, consider a system where a number of patients may be brought back on a weekend afternoon who do not strictly meet the after hours parameters. An example of this would be a deformed wrist fracture: Imaging can wait until morning, but should not wait for two days.
Trauma imaging
Portland is designated as an Urgent Care Service in Victoria’s Trauma system. It is tasked with rapidly assessing and stabilizing trauma patients and then moving them quickly to definitive care. Delayed diagnosis of traumatic injury, especially head injury or occult bleeding increases the likelihood of an adverse outcome.
Urgent radiology is indicated for
• Any trauma meeting major trauma criteria
• Head injury with any of the following
– Focal neurology
– Glasgow Coma Score < 14 (even if possibly due to intoxication)
– Severe headache
– Anticoagulant use (will need rescan at 24 hours also)
• Neck injury with any of the following
– Focal neurology
– Severe neck pain
– Inability to maintain c-spine precautions due to poor patient compliance
– Significant patient discomfort due to hard collar when delay in imaging is likely to be many hours.
• Chest trauma with any of the following
– Respiratory distress
– Hypoxia
– Significant pain
– Significant chest wall or sternal tenderness
• Abdominal trauma with any of the following
– Rebound or guarding
– Hypotension or tachycardia
– Macroscopic haematuria
• Pelvic trauma with
– Pain on pelvic springing
Urgent radiology is seldom indicated for
• Mild symptoms in low impact injury
• Intoxicated patients (GCS14) tolerating the hard collar, where intoxication precludes collar removal, even with a clear CT scan
Respiratory imaging
It can be difficult to diagnose the underlying cause for a patient’s respiratory distress. As treatments can be quite different (diuretics, anticoagulants, bronchodilators), it is important to make the diagnosis as soon as possible. Certain diagnoses (such as pneumothorax or large pleural effusion) can be treated immediately if they can be confirmed.
Urgent radiology is indicated for
• Shortness of breath of uncertain diagnosis with any of the following
– Increased work of breathing
– Tachypnoea
– New hypoxia (saturation < 95%)
• Possible pneumothorax
• Possible thoracic dissection
• Possible large pleural effusion requiring urgent aspiration (and post aspiration film also)
Urgent radiology is seldom indicated for
• Shortness of breath were the patient is not in respiratory distress
– Example: Probable mild to moderate pneumonia
• Shortness of breath where the diagnosis is certain and the patient is improving
– Example: acute asthma
• Possible pulmonary embolus where the patient is stable
– Unless the patient has a high risk of bleeding, the patient can be anticoagulated and imaged the next day
Abdominal imaging
Unless the diagnosis under consideration is likely to require immediate surgery, imaging can be delayed. It is often sensible to discuss the case with surgical staff prior to imaging.
Urgent radiology is indicated for
• Acute abdomen
– Obtain surgical advice. Immediate transfer or operation may be a better option
• Possible organ rupture
• Possible volvulus
• Possible leaking aortic aneurysm
• Possible ectopic pregnancy
• Unfortunately out of hours ultrasound is not available in many rural hospitals. The patient will need to be transferred
Urgent radiology is seldom indicated for
• Abdominal pain with localised abdominal signs
Orthopaedic imaging
Most patients with limb fractures can be made comfortable with splinting and analgesia. They can return the next day for x-ray. Even moderately displaced fractures are unlikely to be operated on after hours. They should also be splinted, but the patient may need to remain in the emergency department until x-ray is available the next morning.
Urgent radiology is indicated for
• Open fractures
• Fractures with significant limb deformity or neurovascular compromise
• Possible dislocation, if immediate relocation is possible
– Patients with recurrent shoulder dislocation may sometimes be relocated without x-ray, and remain in the emergency department for a post reduction film in the morning
• Possible cauda equina syndrome
Urgent radiology is seldom indicated for
• Mild or moderately displaced fractures with little chance of neurovascular problems
• Suspected fractures
Neurological imaging
Urgent radiology is indicated for
• Cerebrovascular accident with any of the following
– Time since symptom free < 3 hours
– Possible intra-cerebral bleed
– Example: associated anticoagulation, hypertension, headache
– GCS < 14
– Deterioration
• Focal seizures
• Prior to lumbar puncture
– Discuss with consultant staff. CT is occasionally not needed
Urgent radiology is seldom indicated for
• Transient ischaemic attack, if symptoms resolved
• Post seizure, if patient is returning to normal GCS
• Syncope, without focal neurology or abnormal vital signs
Other imaging
In general, patients being transferred to intensive care should not have their imaging delayed. If a patient requires urgent transfer for surgery, but that cannot be arranged until imaging results are known, imaging may have to be performed out of hours.
Urgent radiology is indicated for
• Patients being transferred to a critical care bed or for urgent surgery
– Example: post central venous line placement
• Patients requiring anticoagulation, but require exclusion of bleeding
– Example: Possible pulmonary embolus and altered mental state – exclude intracerebral bleed
Urgent imaging is seldom required for
• Possible acute coronary syndrome, if chest is clear and the patient is not being transported
• Peripheral foreign bodies
Dr Tim Baker